 By Carol Gray, LMT, CST, RPYT, ERYT-200
By Carol Gray, LMT, CST, RPYT, ERYT-200
This is part six of the six-part Stuck Baby Series. In part one, My Baby Dropped!, I explain why engagement is pathology. In part two, Why Did My Baby Get Stuck?, I describe the maternal factors that cause babies to get stuck. Part three is Fetal Factors: How Babies Get Themselves Stuck. Part four explores Fetal Constraint: How Culture Immobilizes Babies. Last week, in part five, I looked at How Fetal Constraint Affects Labor and Birth. Today I’m going to describe how fetal constraint or lack of Optimal Fetal Positioning adversely affects the babies themselves — the things we notice at birth and beyond.
The Subtle Things
I see mostly medically normal babies in my bodywork practice. ALL of these babies need some hands-on help. The babies I’ve seen over the years who have needed hands-on help are the ones who drove me to study and practice Craniosacral Therapy. My infant bodywork story is here. MamaSpace Yoga’s birth story is here.
I am a relentless fine-tuner of babies. I’m passionate about doing what I can to insure that, as babies grow, they will be comfortable in their bodies — for life.
Many of the babies I see have:
- Subtle asymmetries (torsions, twists and lateral flexion patterns)
- Feeding difficulties
- Digestive issues
- Sleep problems
- Colic
- Autonomic nervous system dysregulation (extra-fussy, cranky baby)
They have issues that would never interest a neurologist. Yet, they don’t seem to be wired up exactly right. These babies don’t have conditions that would respond to drugs or surgery so their pediatricians deem them normal. Their parents seek help because they know something is wrong.
A Twisted Baby
Thi s baby is a great example of the ones I typically see for bodywork. In my description below, I only describe the things we can actually see with our eyes. As a bodyworker I notice additional things with my hands. The baby’s movements and behavior provide information. The parent/care-giver’s observations also factor into a complete baby assessment.
s baby is a great example of the ones I typically see for bodywork. In my description below, I only describe the things we can actually see with our eyes. As a bodyworker I notice additional things with my hands. The baby’s movements and behavior provide information. The parent/care-giver’s observations also factor into a complete baby assessment.
Here’s what I notice about this baby: Her head rotates to her right. Her left ear tips toward her left shoulder There is significant tension between her brows. Her right eye looks smaller than her left eye. Her nose curves to the right. She has a deep crease between her nose and mouth on the right side, but not on the left. Her yawn is asymmetrical. Her tongue rests mostly on the left side of the floor of her mouth. There is blanching and tension on the left side of her chin. I notice shoulder tension on both sides that makes her neck seem to disappear. I would guess that she has a more difficult time nursing from her parent’s right breast because her neck and shoulders naturally twist in the opposite direction. I’d also wager that she has sub-optimal tongue mobility — another barrier to breastfeeding.
When I look closer I can see that her head twists to her right while her pelvis twists to her left. This creates a spiral shape in her torso. I assume that she got normal embryonic cell allocation on both sides of her body. But in various locations, her body structures have developed asymmetrically because she couldn’t move normally in utero. She looks reasonably calm. She’s yawning and her hands are relaxed. Nonetheless, I would bet that she also has some autonomic nervous system dysregulation that we’re not seeing in the photo.
While they can be addressed therapeutically, structural asymmetries don’t just go away on their own. Over time, babies (or their caregivers) compensate for these things. For example, if this baby has a difficult time transferring milk from the breast or if nursing causes nipple damage for the parent, the common solution to the problem is to offer a bottle. While this may get milk into a baby, the underlying problem has not been addressed. When this baby learns to sit and stand on her own, she will do whatever it takes to keep her eyes level with the horizon and her feet pointing in the same direction as her face. A lot of twisting and turning between her feet and her eyes will occur to make these things happen. This is how lifelong postural and movement patterns are established. It’s the setup for certain arrays of aches, pains and injuries — for life.
Primitive Reflexes
 In my world, lots of people are talking about primitive reflex integration. Reflex integration is the process that causes reflexes we have developed in utero to gradually extinguish. This is supposed to happen as they are replaced by coordinated, voluntary movements. When it doesn’t go well, we see sensory and developmental problems for older babies, children and adults. Repairing reflex integration failure can make huge quality-of-life improvements for children and adults who have these issues. Let’s look at the Rooting Reflex. When a baby’s cheek is touched they turn their head toward the touch and open their mouths. If that touch came from a nipple, they are on-track to get fed. If an adult turns their head and opens their mouth every time their cheek gets touched, it’s a problem. The reflex is supposed to be temporary.
In my world, lots of people are talking about primitive reflex integration. Reflex integration is the process that causes reflexes we have developed in utero to gradually extinguish. This is supposed to happen as they are replaced by coordinated, voluntary movements. When it doesn’t go well, we see sensory and developmental problems for older babies, children and adults. Repairing reflex integration failure can make huge quality-of-life improvements for children and adults who have these issues. Let’s look at the Rooting Reflex. When a baby’s cheek is touched they turn their head toward the touch and open their mouths. If that touch came from a nipple, they are on-track to get fed. If an adult turns their head and opens their mouth every time their cheek gets touched, it’s a problem. The reflex is supposed to be temporary.
Lately, I’ve become more interested in the question of what happens when the primitive reflexes never develop optimally in the first place. We’re back to the Rooting Reflex. If this reflex is absent or weak, it makes feeding harder for a baby. The parent has to assume part of what normally would be the baby’s role in order to get the baby fed.
What happens when the reflexes are established, but don’t have the opportunity to stimulate muscle development and strengthening due to fetal constraint? In the case of the Rooting Reflex, it may be present, but for a baby who couldn’t, for example, turn their head to the left in utero, the muscles that should turn the head to the left are weak after birth. This baby would have harder time feeding at the parent’s right breast.
If you want to learn more about primitive reflex development, I give a simple description in this article. The reflexes, themselves, are responsible for strengthening babies’ muscles in utero. More importantly, it endows babies with the skills they need to get born and survive life on the outside while they are learning to voluntarily move their bodies. One important part of a newborn exam conducted by a midwife, doctor or nurse is to touch babies in certain ways to licit these reflexes. If they are absent or abnormal, further investigation is warranted.
Really, the only reason we have brains is to move our bodies. All necessary elements for life require movement. There are no exceptions to this rule.
I discuss and demonstrate primitive reflexes at work in this video called Infant Unwinding.
Cranial Nerve Dysfunction
 Cranial nerves emerge from the brain stem. They are responsible for sensation, function and movement of certain body parts – especially in the head and neck. They affect posture, tongue function, vision, eye movements, sense of smell, hearing, digestion and sense of taste. The muscles that drive suck/swallow/breathe coordination depend on appropriate cranial nerve function. Cranial nerves also stimulate facial expression and vocalization — the primary tools of social engagement.
Cranial nerves emerge from the brain stem. They are responsible for sensation, function and movement of certain body parts – especially in the head and neck. They affect posture, tongue function, vision, eye movements, sense of smell, hearing, digestion and sense of taste. The muscles that drive suck/swallow/breathe coordination depend on appropriate cranial nerve function. Cranial nerves also stimulate facial expression and vocalization — the primary tools of social engagement.
Cranial nerve dysfunction is associated with asymmetries. Sometimes this happens when a baby is stuck in utero — especially for a long time in an asymmetrical position. It can also happen if the baby has a rough birth, which, of course, can be caused by fetal constraint.
When fetal constraint affects the cranial base, it can compress cranial nerves. This may inhibit normal sensations, movement and function. Compromised cranial nerves will ultimately cause more asymmetries in the body. Here’s an example: A baby has cranial base compression that affects spinal accessory nerve on one side. This causes weakness in certain neck muscles on that side. Consequently, the baby is born with a head turning preference. Over time, the body will compensate in the opposite direction in order to keep the eyes level and straight ahead. This causes another imbalance.
Cranial nerve dysfunction causes autonomic nervous system and emotional dysregulation. These frequently-upset babies seem to be RAW. Their response to typical stimulation is way beyond what we would expect. The baby in this picture is having emotional regulation issues.
Babies (even the dysregulated ones) learn emotional regulation from their parents/caregivers. We regulate them with nurturing, soothing behavior. I’m going to get on my soapbox for a moment. I hear many people say they want their babies to learn to self-soothe. They may ignore their babies’ cries in an attempt to facilitate self-soothing. At some point, babies will stop crying if no one comes to their aid because they will have fallen into a state of despair. Babies don’t actually have the limbic system (feeling brain) support to BEGIN TO LEARN self-regulation and to soothe themselves until they are about three years old. The entire process takes MANY years throughout childhood and young-adulthood as the neocortex (the thinking brain) develops. The developmental timetable can’t be rushed or trained.
The Not-So-Subtle Things
Club Foot
 This baby’s foot & ankle grew this way because they didn’t have the physical space to grow normally. Babies grow into available space.
This baby’s foot & ankle grew this way because they didn’t have the physical space to grow normally. Babies grow into available space.
Club Foot Treatment
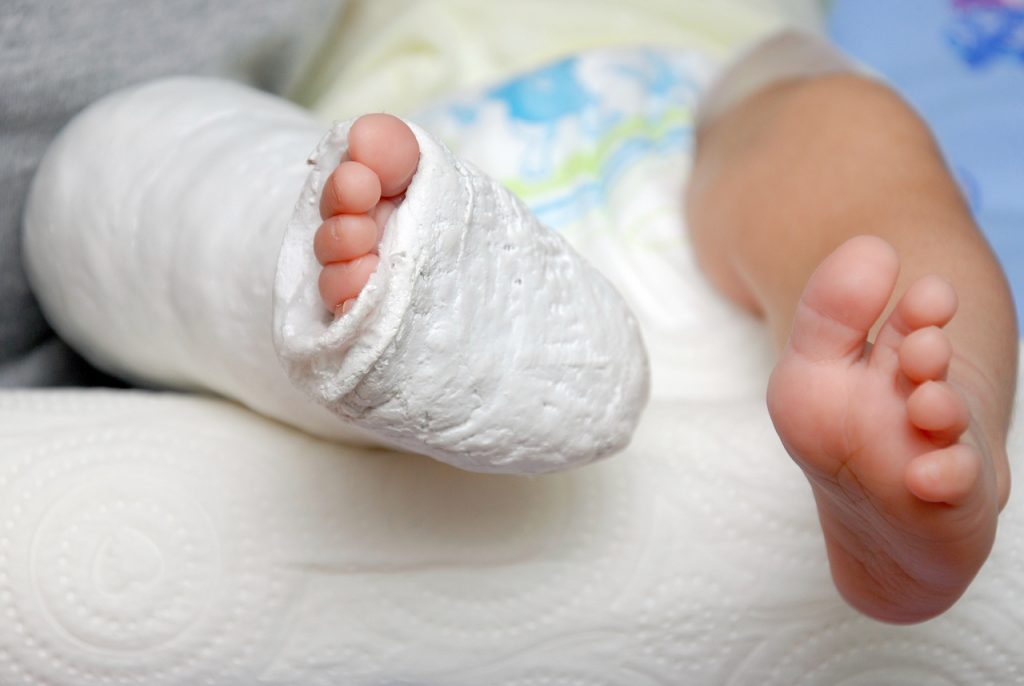 This baby’s club foot is being treated with a series of casts that restrict foot and ankle movement and growth in the undesired direction. The casts allow movement and growth in the desired direction. They are changed frequently to accommodate the baby’s growth and the shape-changes that slowly occur from the casting process. This is another great example of babies growing into available space. If they gestate asymmetrically, it is possible to change things after birth — if corrective measures are applied early and consistently. Growth fuels the change. The rate of human growth generally slows from conception forward (in puberty there is an uptick in growth rate). Babies grow fast, but every day the growth rate slows. Sometimes surgery is required to resolve club foot.
This baby’s club foot is being treated with a series of casts that restrict foot and ankle movement and growth in the undesired direction. The casts allow movement and growth in the desired direction. They are changed frequently to accommodate the baby’s growth and the shape-changes that slowly occur from the casting process. This is another great example of babies growing into available space. If they gestate asymmetrically, it is possible to change things after birth — if corrective measures are applied early and consistently. Growth fuels the change. The rate of human growth generally slows from conception forward (in puberty there is an uptick in growth rate). Babies grow fast, but every day the growth rate slows. Sometimes surgery is required to resolve club foot.
Torticollis
 Torticollis is the most frequently undiagnosed problem I encounter in my bodywork practice. It is a key player in positional plagiocephaly (flat spot on one side of a baby’s head). I wrote about flat spots here.
Torticollis is the most frequently undiagnosed problem I encounter in my bodywork practice. It is a key player in positional plagiocephaly (flat spot on one side of a baby’s head). I wrote about flat spots here.
It used to be called wry neck syndrome. Some babies appear to favor rotating their heads more to one side than the other. Or, they may have a lateral flexion preference (a head tilt to one side). It’s common to see a baby who rotates their head one way while laterally flexing it the other way. That’s what the baby in this picture is doing.
Torticollis looks like a neck thing, but it is actually happening throughout the torso. It has potential to extend into the floor of the mouth and adversely affect tongue mobility and feeding. Even if the restrictions don’t extend into the mouth, these twisted babies may simply have a difficult time breastfeeding on one side or in certain positions. The twist can also extend into the cranial base contributing to cranial nerve dysfunction due to compression (described above). Of course, the entire spine and pelvis are also involved. Could this affect a female baby’s future experience of pregnancy and her own baby’s gestation, birth and development? I say yes, the potential is there.
Hip Dysplasia
 Lack of fetal mobility causes hip dysplasia. The hip joint is a ball and socket joint. The socket part of the hip joint is called the acetabulum. During gestation it starts out shallow. The ball at the top of the baby’s thigh bone – or femoral head – is supposed to press into the acetabulum causing it to form a cup around the ball. If this doesn’t happen, the joint remains too shallow and is unstable.
Lack of fetal mobility causes hip dysplasia. The hip joint is a ball and socket joint. The socket part of the hip joint is called the acetabulum. During gestation it starts out shallow. The ball at the top of the baby’s thigh bone – or femoral head – is supposed to press into the acetabulum causing it to form a cup around the ball. If this doesn’t happen, the joint remains too shallow and is unstable.
Hip dysplasia is more common among babies who are stuck in a frank breech position. Frank breech is where a baby is jackknifed with their pelvis jammed into the maternal pelvis and their feet near their faces. This position pulls the femoral head away from the acetabulum. Any baby can get stuck in a position that creates the conditions for hip dysplasia. Frank breech isn’t the only way.
Some things we do with our babies after they are born can cause hip dysplasia, too. I’ll write about that next week.
Hip Dysplasia Treatment
 The treatments for hip dysplasia include casting or special harnesses that hold the legs in a “froggie” position. Sometimes surgery is required to stabilize the joints.
The treatments for hip dysplasia include casting or special harnesses that hold the legs in a “froggie” position. Sometimes surgery is required to stabilize the joints.
Scoliosis
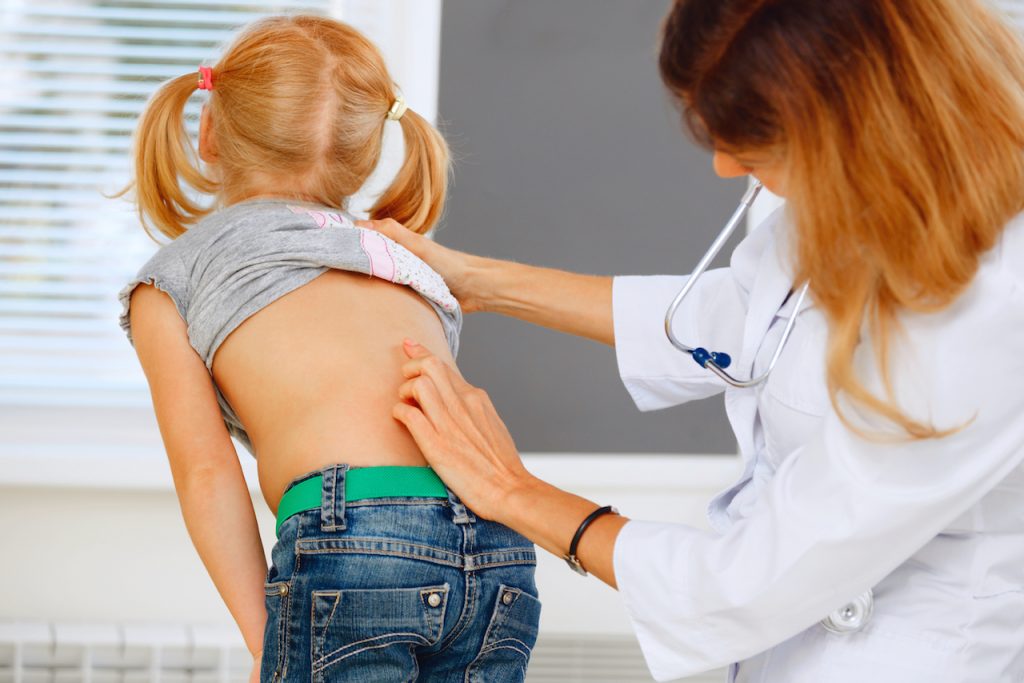 Lack of fetal mobility causes scoliosis. Scoliosis is usually diagnosed in school aged children. I assert that it has been there all along – since before birth. We don’t usually SEE it in babies because they haven’t yet spent time standing and walking in gravity. It’s the upright position in gravity and that drive to keep the eyes facing forward and level with the horizon that cause the compensations for scoliosis to appear. These compensations are what we actually see – the muscular length and strength imbalances on either side of the spine and the apparent lateral curvature of the spine – which, incidentally, is actually a rotation.
Lack of fetal mobility causes scoliosis. Scoliosis is usually diagnosed in school aged children. I assert that it has been there all along – since before birth. We don’t usually SEE it in babies because they haven’t yet spent time standing and walking in gravity. It’s the upright position in gravity and that drive to keep the eyes facing forward and level with the horizon that cause the compensations for scoliosis to appear. These compensations are what we actually see – the muscular length and strength imbalances on either side of the spine and the apparent lateral curvature of the spine – which, incidentally, is actually a rotation.
I believe that scoliosis is a torsion in the deep structures anterior to the spine – structures like the mediastinum, the root of the mesentery and the things we call ligaments that are actually folds of peritoneum (the lining of the abdominal and thoracic cavities). They attach thoracic and abdominal organs to adjacent structures. These torsions develop in utero. Some people say scoliosis runs in families. I say the big baby who gestates in a woman with a short torso is what runs in families. More on that below.
A Personal Scoliosis Story
 This is my husband, Steve, and our dog, Roy. Steve was diagnosed with scoliosis as a small child. He had what’s commonly called the c-curve variety. When I looked at his back while he was standing or moving it was obvious. He said that in his yoga practice he could twist in one direction – the direction of his rotation – with ease. When he tried to twist in the opposite direction of his rotation, he felt like he was spring-loaded. He could barely twist that way.
This is my husband, Steve, and our dog, Roy. Steve was diagnosed with scoliosis as a small child. He had what’s commonly called the c-curve variety. When I looked at his back while he was standing or moving it was obvious. He said that in his yoga practice he could twist in one direction – the direction of his rotation – with ease. When he tried to twist in the opposite direction of his rotation, he felt like he was spring-loaded. He could barely twist that way.
Seven years ago Steve had a liver transplant. Now his scoliosis is completely gone. It’s obvious to me that it’s completely gone when I look at him while he’s standing and moving. He also reports equal twisting ability in his yoga practice.
Naturally, this got my attention. I asked one of the surgeons on the transplant team about it. I wondered if they had cut out his old liver and then somehow the support ligaments re-positioned themselves before they sewed the new liver into place. The doctor told me that they only attach the blood vessels and the ducts. The rest of it scars into place. Steve had resumed his yoga practice post transplant before the doctors said he should. That probably helped him gain maximum mobility for his new liver and the adjacent structures. I’m glad he didn’t resume running sooner than they had advised.
Steve was a nearly 10 pound baby who was 21.5” long. He developed as a first baby in the womb of a woman with a short torso who was 5’1” tall. I contend his scoliosis was due to lack of mobility in utero.
That’s it for this week. Next week will be an add-on to this series: Things We Do After Birth That Prevent Babies From Moving. Until then…
Love,
Carol
About Carol Gray
 Carol is the founder and owner of MamaSpace Yoga. She has been a therapeutic bodyworker in private practice for over 31 years. She specializes in Craniosacral Therapy for pregnant and postpartum people and infants. Carol has spent years developing hands-on techniques to enhance the mobility in pregnant bodies including the bony pelvis, the abdominal organs, the support structures and lower segment of the uterus. She is proud to have pioneered the integration of this gentle manual therapy into prenatal care, the birth place and postpartum care for birthing parents and babies. The goal is to give babies more room to develop, grow and get born. Her specially-designed yoga classes have grown naturally from the roots of bodywork and yoga.
Carol is the founder and owner of MamaSpace Yoga. She has been a therapeutic bodyworker in private practice for over 31 years. She specializes in Craniosacral Therapy for pregnant and postpartum people and infants. Carol has spent years developing hands-on techniques to enhance the mobility in pregnant bodies including the bony pelvis, the abdominal organs, the support structures and lower segment of the uterus. She is proud to have pioneered the integration of this gentle manual therapy into prenatal care, the birth place and postpartum care for birthing parents and babies. The goal is to give babies more room to develop, grow and get born. Her specially-designed yoga classes have grown naturally from the roots of bodywork and yoga.
Carol has dedicated her professional life to supporting expectant and new families by promoting gentle aware birth. She attended births for over 35 years – at first as a doula and from 2000 to 2012 as a midwife. She has since retired from attending births in order to focus on practicing and teaching CST and prenatal yoga. Her many years as a birth worker have forever changed her and her worldview. Those experiences remain an integral part of who she is as a therapist and teacher.
Carol is the founder and director of the The Carol Gray Center for CST Studies®. She teaches high-quality, small group classes that are appropriate for bodyworkers, birth attendants and other health professionals. She is approved by the National Certification Board for Therapeutic Massage and Bodywork (NCBTMB) as a continuing education approved provider.

