By Carol Gray, LMT, CST, RPYT, ERYT-200
This is the fourth installment of the stuck baby series. Last week I described the fetal factors (ways babies get themselves stuck). The week before I discussed maternal factors. Three weeks ago I covered engagement and explained why it’s pathology. Next week I’ll go over how fetal constraint affects labor and birth. Stay tuned!
Today I’m going to discuss cultural factors that reduce babies’ opportunities to move in utero and cause them to get stuck. This is the category we can actually do something about because the factors are under our conscious control — if we know enough and if we care care enough.
The persistent erroneous belief that engagement/Fixation is normal
 This is a biggie. Most of the industrialized world still believes that engagement/fixation is normal. I believe it’s pathology – far from optimal fetal positioning. This pathology is on the increase. The fact that people THINK it’s normal contributes to the problem. If we think it’s normal we are disinclined to do anything about it. It is more common than it used to be. But common is NOT the same as normal.
This is a biggie. Most of the industrialized world still believes that engagement/fixation is normal. I believe it’s pathology – far from optimal fetal positioning. This pathology is on the increase. The fact that people THINK it’s normal contributes to the problem. If we think it’s normal we are disinclined to do anything about it. It is more common than it used to be. But common is NOT the same as normal.
Did you know that some scheduled cesareans, sadly, are done for lack of engagement late in pregnancy? Yep. Some pregnant people are told by their doctors that things are not looking good for a vaginal birth because the baby has failed to engage/get stuck by 36 weeks. Is this grooming for a scheduled cesarean that will happen during business hours on a weekday? Call me cynical.
CARE PROVIDERS WHO DON’T PALPATE
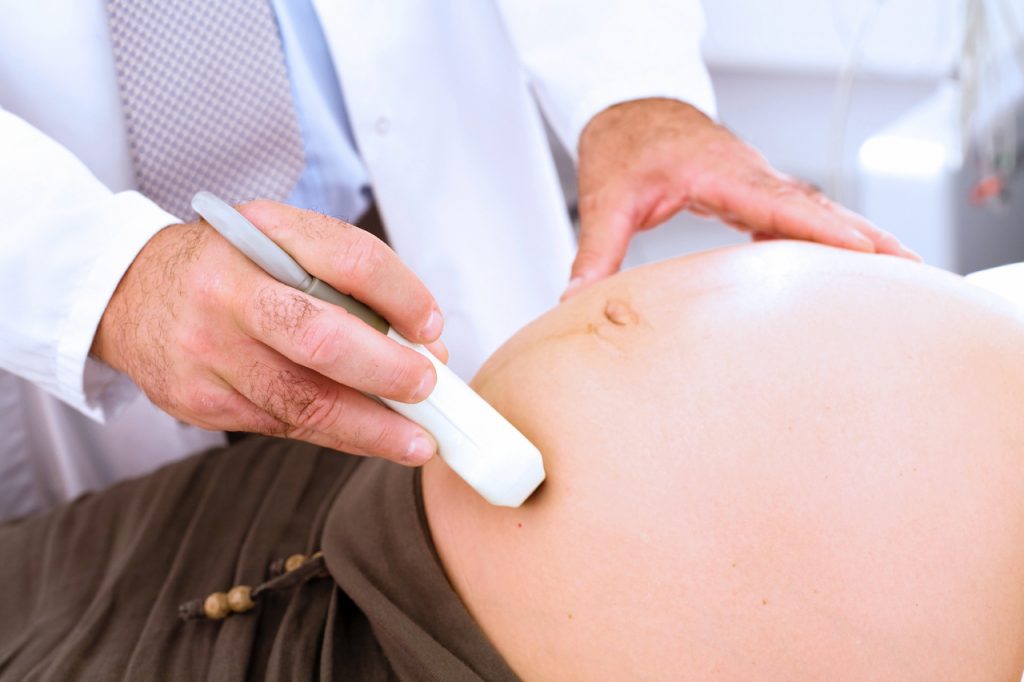 This is going to be a rant. So hang on. When pregnant people visit their doctors and many hospital-based midwives for prenatal visits, their providers don’t necessarily palpate the position of the baby. They certainly don’t do anything to enhance the positioning of the baby during these visits. They rely — for the most part — on ultrasound. They will usually order an ultrasound at 36 weeks to assess the baby’s position and also look at some other things. Rarely do they check at a prenatal visit for anything beyond whether the baby is breech or not. Any position that is not head down is considered breech. This includes a wide variety of positioning possibilities.
This is going to be a rant. So hang on. When pregnant people visit their doctors and many hospital-based midwives for prenatal visits, their providers don’t necessarily palpate the position of the baby. They certainly don’t do anything to enhance the positioning of the baby during these visits. They rely — for the most part — on ultrasound. They will usually order an ultrasound at 36 weeks to assess the baby’s position and also look at some other things. Rarely do they check at a prenatal visit for anything beyond whether the baby is breech or not. Any position that is not head down is considered breech. This includes a wide variety of positioning possibilities.
We know that babies need to have their chins tucked and their faces toward the parent’s back. The center of the lambda (also called the posterior fontanelle or posterior soft spot ) should be pointing toward the parent’s pelvic outlet for things to fit best. Do they check for this? Nope. Why is it like this? One reason is that obstetricians are also surgeons. It doesn’t really matter to them if the baby is growing in an ideal position or not because they can always do a cesarean surgery.
Cesarean birth is safer than it used to be and is linked to better outcomes for doctors and hospitals in medical malpractice suits. Even though it is more dangerous than a vaginal birth, the general public is pretty OK with it. In fact, one of the doctors’ reasons to do this 36-week ultrasound is to determine whether and when to schedule a cesarean for a breech position. That’s how they look at it.
Another reason is that the level of palpation skills required to determine nuances of baby positions are rarely taught in medical schools or obstetric residency programs anymore. Some doctors cannot determine with their hands even the most basic element of a baby’s position: Is the head up or down? Is it possible to figure out with our hands whether a baby’s head is up or down, whether their chins are tucked and whether they have their backs facing the front of their parent’s body? Of course it is. I did it all the time as a midwife. If people are trained and get some practice, palpation is just as accurate as ultrasound for determining fetal position. It costs less, too.
I’m frustrated by the number of people I see for the first time in my bodywork practice at 38 or 39 weeks. They say their 36 week ultrasound showed the baby to be breech and ask me what I can do for them. Of course, I do make enough space for some of these babies to turn on their own, but I also think to myself, “Where were you a few weeks ago when we could have done more about this?” Surely, these babies didn’t decide to turn breech on the way to the ultrasound appointment.
WHY DON’T THEY JUST TURN THE BABY?
 Several years ago one of my midwife colleagues hosted a group of midwives from Central America and Mexico during a Midwives Alliance of North America conference that was held in Portland. In those days the mechanism for foreign language interpretation in the general sessions was to group non-English speakers at the same table as their translator. My colleague is a fluent Spanish speaker and was interpreting for this group during the conference.
Several years ago one of my midwife colleagues hosted a group of midwives from Central America and Mexico during a Midwives Alliance of North America conference that was held in Portland. In those days the mechanism for foreign language interpretation in the general sessions was to group non-English speakers at the same table as their translator. My colleague is a fluent Spanish speaker and was interpreting for this group during the conference.
This particular session was about managing breech birth. As she translated, the women at her table erupted. They all started talking at once. They said things like, “You allow births like that in this country? Why don’t they just turn the baby? We always turn the baby. We check the baby’s position every time and just turn the babies if they are breech. We never have breech birth”
I wrote about the Sobada — a traditional abdominal massage given to pregnant people to help their babies assume ideal positions for birth — in this post.
External Cephalic Version
 What we do in the US is external cephalic versions at 36-42 weeks. These are rough-handed procedures. Doctors typically schedule ONLY a half hour to turn a baby. People tell me it’s painful and stressful. Doctors typically schedule external cephalic versions no earlier than 36 weeks because there is a risk that the labor will have to be induced due to ruptured membranes caused by the roughness of the procedure. There is also a small risk that an emergency cesarean will be needed due to cord compression or placental abruption. Of course, the rough-handedness and speed at which the procedure is done greatly contributes to these risks.
What we do in the US is external cephalic versions at 36-42 weeks. These are rough-handed procedures. Doctors typically schedule ONLY a half hour to turn a baby. People tell me it’s painful and stressful. Doctors typically schedule external cephalic versions no earlier than 36 weeks because there is a risk that the labor will have to be induced due to ruptured membranes caused by the roughness of the procedure. There is also a small risk that an emergency cesarean will be needed due to cord compression or placental abruption. Of course, the rough-handedness and speed at which the procedure is done greatly contributes to these risks.
By the way, guess which babies are hardest to turn? That’s right. The ones whose presenting parts are engaged – I Mean FIXATED – in the maternal pelvis. The pregnant person in this picture is already in pain and they’ve just barely gotten started with the procedure.
The Gentle Way — The Midwife Way
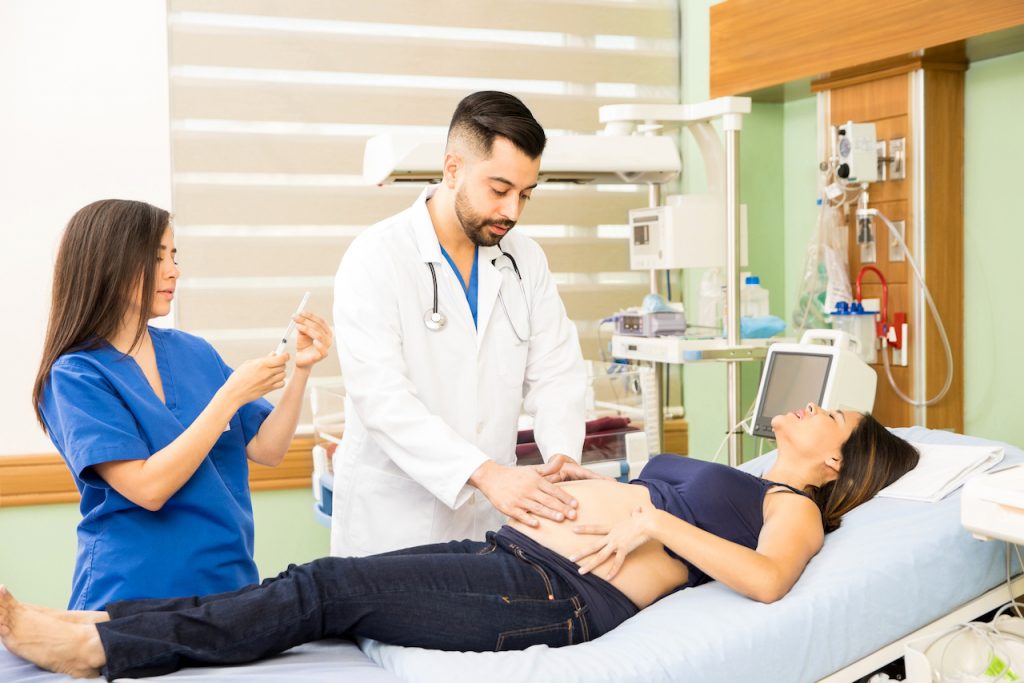
 Here’s a picture of a midwife visiting a pregnant client. She’s carefully palpating the position of the baby and may even give a little nudge one way or the other to encourage the baby to assume a nuanced good position. It makes sense to me that providers should be palpating the position of the baby at each visit. That way if the baby is in a less than ideal position something could be done about it – such as GENTLY maneuvering the baby into a better position and encouraging parents to alter their postural and movement activities EARLY while the baby still has more buoyancy and room to move. But, mostly, that’s not how it’s done in the US.
Here’s a picture of a midwife visiting a pregnant client. She’s carefully palpating the position of the baby and may even give a little nudge one way or the other to encourage the baby to assume a nuanced good position. It makes sense to me that providers should be palpating the position of the baby at each visit. That way if the baby is in a less than ideal position something could be done about it – such as GENTLY maneuvering the baby into a better position and encouraging parents to alter their postural and movement activities EARLY while the baby still has more buoyancy and room to move. But, mostly, that’s not how it’s done in the US.
I know a few homebirth midwives and naturopathic physicians in my community who specialize in helping babies turn with gentle hands-on maneuvers. It can take an hour or two of hands-on time to get the job done. Why does it take that long? Because it takes that long. 20-30 minutes for the entire appointment is a ridiculously unrealistic amount of time for this procedure. Our weddedness to the industrial model of medicine is one of the causes of stuck babies. Childbirth is actually a consumer-driven industry in the US and other industrialized countries. We can demand something different.
Seated Occupations for Pregnant People
 I wrote about this two weeks ago in the post called My Baby Dropped!
I wrote about this two weeks ago in the post called My Baby Dropped!
Most pregnant people in industrialized countries work outside of the home — more than 70% in the US. 50 years ago in the US more than 50% of jobs required at least moderate physical activity. Now fewer than 20% require it. This trend is growing in all industrialized countries. Seated occupations are the norm. I do love the way the person in this picture is sitting, by the way — on a ball with an anterior pelvic tilt. I hope they get up and walk around frequently.
Not everyone has a nice, seated work set-up like the one in this photo. I suspect that during the pandemic, with the sudden shift to working from home, people are more likely sitting at the kitchen table with a posterior pelvic tilt. I imagine keyboards and screens at the wrong height — at least from an ergonomic perspective. I can also imagine people slouching on the couch with a tablet or laptop, semi-reclined with a posterior pelvic tilt. It makes me cringe.
Baby-Lifting Garments

 This is something we usually DON’T choose in the US, Canada and most of Europe — probably other places, too. It’s a baby-lifter.
This is something we usually DON’T choose in the US, Canada and most of Europe — probably other places, too. It’s a baby-lifter.
Let’s start with the one on the left. It may seem counter-intuitive because it looks to be — and is — wrapped snugly around the pregnant belly in this picture. However, notice that the thickest part of the fabric is actually below the belly. That’s the tight part. The tight, supportive part is high in the back and low in the front. This serves to prevent the baby from fixating deeply into the maternal pelvis. Instead, this baby gets to spend more time in the upper, more roomy part of the pelvis. When babies aren’t stuck down low, they can move more.
A baby-lifter also prevents and provides fantastic relief from low back and pelvic pain during pregnancy. Many cultures have a version of this garment. In the US, if we use one at all, we tend to favor the industrial model shown in the photo on the right.
It surprises me that when I recommended one of these garments (either the homemade one shown on the left or the store-bought one shown on the right) many people have never heard of them. I think ALL pregnant people should use one. I repeat, all pregnant people. The one complaint I hear about these is that they tend to be uncomfortable if the wearer is seated for a long time. There is a message in that…
Other Things We Choose/Love That Get Our Babies Stuck
- Screens — as in sit in one place for a long time
- TV — as in sit in one place for an even longer time
- Automobiles — we can’t stand and walk around in them and they force us into a posterior pelvic tilt when we sit
- Epidural anesthesia for childbirth — also a choice that can get a baby stuck during the birth process. Although, I have on occasion seen a seemingly stuck baby make their way out after an epidural is administered. This is due to a little more maternal space associated with iliopsoas flaccidity (look it up).
- It’s still a common belief that pregnant people are fragile and shouldn’t be active or exert themselves “too much” because something is bound to go wrong.
That’s it for this week. Next week I’ll describe the problems caused by stuck babies. There are many.
Love,
Carol
P.S. If you were keeping track of how many maternal factors vs fetal factors vs cultural factors conspire to get babies stuck, I would wager that cultural factors are the winners. Many of the maternal factors are caused or exacerbated by the cultural factors. The babies are relatively innocent in this — as it should be.
About Carol Gray
 Carol is the founder and owner of MamaSpace Yoga. She has been a therapeutic bodyworker in private practice for over 31 years. She specializes in Craniosacral Therapy for pregnant and postpartum people and infants. Carol has spent years developing hands-on techniques to enhance the mobility in pregnant bodies including the bony pelvis, the abdominal organs, the support structures and lower segment of the uterus. She is proud to have pioneered the integration of this gentle manual therapy into prenatal care, the birth place and postpartum care for birthing parents and babies. The goal is to give babies more room to develop, grow and get born. Her specially-designed yoga classes have grown naturally from the roots of bodywork and yoga.
Carol is the founder and owner of MamaSpace Yoga. She has been a therapeutic bodyworker in private practice for over 31 years. She specializes in Craniosacral Therapy for pregnant and postpartum people and infants. Carol has spent years developing hands-on techniques to enhance the mobility in pregnant bodies including the bony pelvis, the abdominal organs, the support structures and lower segment of the uterus. She is proud to have pioneered the integration of this gentle manual therapy into prenatal care, the birth place and postpartum care for birthing parents and babies. The goal is to give babies more room to develop, grow and get born. Her specially-designed yoga classes have grown naturally from the roots of bodywork and yoga.
Carol has dedicated her professional life to supporting expectant and new families by promoting gentle aware birth. She attended births for over 35 years – at first as a doula and from 2000 to 2012 as a midwife. She has since retired from attending births in order to focus on practicing and teaching CST and prenatal yoga. Her many years as a birth worker have forever changed her and her worldview. Those experiences remain an integral part of who she is as a therapist and teacher.
Carol is the founder and director of the The Carol Gray Center for CST Studies®. She teaches high-quality, small group classes that are appropriate for bodyworkers, birth attendants and other health professionals. She is approved by the National Certification Board for Therapeutic Massage and Bodywork (NCBTMB) as a continuing education approved provider.


