 By Carol Gray, LMT, CST, RPYT, ERYT-200
By Carol Gray, LMT, CST, RPYT, ERYT-200
The word “emergency” used to ONLY apply to childbirth. The baby emerges, get it?
Two (Three) Kinds of Cesareans
Lately, I have been hearing an emergent theme in the stories people have been sharing with me about their cesarean births. They divide them into two categories – planned and emergency. Often a parent will say to me that their cesarean birth was not planned. It was an emergency. Yet, when I hear the details of the story it almost always falls into the third and largest category – the unplanned cesarean. It is really a story about a failed induction, a less-then-ideally positioned baby who fails to descend (and emerge), a baby who wasn’t coping well with labor contractions, but didn’t need to come out RIGHT NOW, etc.
The Story
I’m concerned that people are somehow believing that their births were an emergency when they actually weren’t. Can these stories lead to unnecessary emotional trauma for parents? I think this can be especially weird for the child who grows up to believe that they almost died during an “emergency” birth when the facts are actually something like “failure to progress” or a doctor who wanted to both get paid for the birth and go home at a reasonable hour.
“You’re Going to Sleep Now. We’ll Take Good Care of You and Your Baby.”
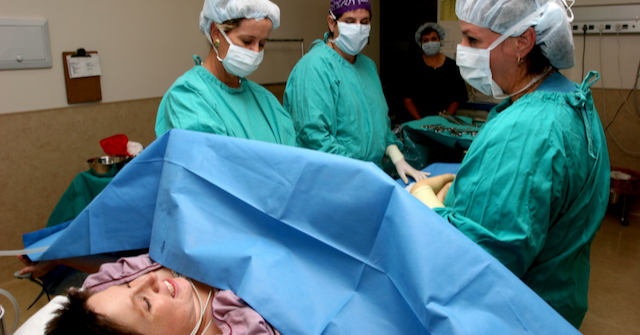
A true emergency or “crash” cesarean happens with general anesthesia and the baby is out in less than 10 minutes from the time the decision is made to do the surgery. This happens for things like placental abruptions and cord prolapses – true life-threatening emergencies. These are very rare occurrences.
Planning For the Unexpected Cesarean Will Not Cause It
We all know the cesarean rate is high. In the US, a birthing parent’s odds of having surgery to get their babies born are approximately 1 in 3. Cesarean birth is NOT caused by planning in advance how to cope with it when it happens. I think that when families do some advance planning they will have better experiences. They may feel better about their surgical births and may be less likely to define them as emergencies when the facts don’t support the label.
Planning Strategies for Parents and Support People:
Discuss and Agree
In my experience (I’ve done some primary research on this) birthing parents will have a better, quicker and more complete recovery from a cesarean birth if they have some time to process and agree with the decision to do the cesarean birth. When there is no emergency, birthing parents should always ask for a few minutes alone with their partners, doulas and other support people. During that alone time they should discuss all the reasons for and against the decision, identify any lingering questions – particularly about other options – and (after getting answers to lingering questions) come to agreement that surgery is the best option. It can make a huge difference in parents’ emotional recovery if they feel afterwards that they had ample time to process the decision and agree with it.
Support For the Birthing Parent and the Baby
I think it is important for more than one support person to suit up to go into the OR – even when they only let one person in at a time (two at a time is better and can often be negotiated). If there is something happening with a baby that requires an immediate trip to the nursery, the child’s other parent (or other designated person) will likely (should) go with the baby. This leaves the birthing parent high and dry support-wise while their surgery is completed. In this case the extra person (already by the birthing parent’s side or waiting just outside the door) can stay with the birthing parent or enter the OR and support them. They can sometimes ferry information and phone pictures of baby to parent and of parent to baby.
The Blessed Event
I think it is good for someone (birthing parent, their partner or the doula) to remind hospital staff that this is one family’s blessed event. I tell hospital staff that the family would like conversation (other than what is needed for staff to communicate with each other about the surgery) to be kept to a minimum. Most folks don’t really want to hear, during the birth of their child, what the anesthesiologist’s teenage son did with the family car the night before.
My Baby
I tell the baby’s other parent or the birthing parent’s support person to follow the baby across the room once the baby is born. They should talk to the baby and touch the baby. I tell the other parent that even if staff are doing stuff to the baby and there are several hands on the baby, their hands and voice should be there, too. This is comforting and reassuring to babies. I have a favorite memory of a dad in the OR who caused nurses to attempt several weighings because he kept touching his baby while the child was on the scale. I saw the nurses roll their eyes every time they had to zero out that scale and start over. I was very proud of this dad.
The Natural Cesarean
Parents can request (with varying degrees of success – depending on the hospital) things like low lights for the emergence of the baby, slow release of amniotic fluid, delayed cord clamping and skin to skin in the OR. Hospital birth is actually to some degree a consumer-driven activity. When more parents request these things, we are more likely to see them happen.
The Little Things That Count
Little things like dropping the screen so the birthing parent can see their babies emerge (they can’t see the actual incision over the baby bump while lying on their backs), allowing the parents to be the ones to discover and declare the sex of the baby (if they don’t already know), the “right” music playing in the OR and one hand free so the birthing parent can easily touch their baby can also make a big difference in the cesarean experience.
Parent/Baby Communication
Last, I ask surgeons or nurses to tell us when they are going to make the first incision, when they are going to make the incision into the uterus and when they will lift the baby out. That way the birthing parent can let the baby know in advance what is going on. This is really important for babies, obviously, and also really important for the parents. Parents who have done this have reported to me that they felt calm and centered during the process while they were communicating with their babies in this way.
I hope this gives you some things to think about. In the mean time, let’s do some online prenatal or postpartum yoga together.
About Carol Gray
 Carol is the founder and owner of MamaSpace Yoga. She has been a therapeutic bodyworker in private practice for over 30 years. She specializes in Craniosacral Therapy for pregnant and postpartum people and infants. Carol has spent years developing hands-on techniques to enhance the mobility in pregnant bodies including the bony pelvis, the abdominal organs, the support structures and lower segment of the uterus. She is proud to have pioneered the integration of this gentle manual therapy into prenatal care, the birth place and postpartum care for birthing parents and babies. The goal is to give babies more room to develop, grow and get born. Her specially-designed yoga classes have grown naturally from the roots of bodywork and yoga.
Carol is the founder and owner of MamaSpace Yoga. She has been a therapeutic bodyworker in private practice for over 30 years. She specializes in Craniosacral Therapy for pregnant and postpartum people and infants. Carol has spent years developing hands-on techniques to enhance the mobility in pregnant bodies including the bony pelvis, the abdominal organs, the support structures and lower segment of the uterus. She is proud to have pioneered the integration of this gentle manual therapy into prenatal care, the birth place and postpartum care for birthing parents and babies. The goal is to give babies more room to develop, grow and get born. Her specially-designed yoga classes have grown naturally from the roots of bodywork and yoga.
Carol has dedicated her professional life to supporting expectant and new families by promoting gentle aware birth. She has attended births for over 35 years – at first as a doula and from 2000 to 2012 as a midwife. She has since retired from attending births in order to focus on practicing and teaching CST and prenatal yoga. Her many years as a birth worker have forever changed her and her worldview. Those experiences remain an integral part of who she is as a therapist and teacher.
Carol is the founder and director of the The Carol Gray Center for CST Studies®. She teaches high-quality, small group classes that are appropriate for bodyworkers, birth attendants and other health professionals. She is approved by the National Certification Board for Therapeutic Massage and Bodywork (NCBTMB) as a continuing education approved provider.

